February 22, 2024
3 books · 53 highlights · 3 notes

Exosomes Derived From Schwann Cells Ameliorate Peripheral Neuropathy in Type 2 Diabetic Mice
Wang, Lei
“Schwann cell–derived exosomes communicate with dorsal root ganglia (DRG) neurons”
9:22 AM
“Exosomes Derived From Schwann Cells Ameliorate Peripheral Neuropathy in Type 2 Diabetic Mice”
9:23 AM
“therapeutic effect of exosomes derived from healthy Schwann cells (SC-Exos) on diabetic peripheral neuropathy (DPN)”
9:23 AM
“intravenous administration of SC-Exos to type 2 diabetic *db/db* mice with peripheral neuropathy remarkably ameliorated DPN by improving sciatic nerve conduction velocity and increasing thermal and mechanical sensitivity”
9:23 AM
“SC-Exo treatment reversed diabetes-reduced mature form of miRNA (miR)-21, -27a, and -146a and diabetes-increased semaphorin 6A (SEMA6A)”
9:24 AM
“SC-Exos promoted neurite outgrowth of diabetic DRG neurons and migration of Schwann cells challenged by high glucose”
9:25 AM
“Myelin-forming Schwann cells, the most abundant cells in the peripheral nervous system, interact with axons and blood vessels to regulate peripheral nerve function ([1](javascript:;),[4](javascript:;),[5](javascript:;)). Dysfunction of these interactions contributes to the development of DPN”
10:06 AM
“Exosomes are nanovesicles (30–200 nm) and play a major role in mediating intercellular communication through transferring their bioactive cargo, including miRs, to recipient cells, ultimately regulating recipient cell function”
1:28 PM
“exosomes derived from high-glucose (HG)–challenged Schwann cells promote the development of DPN in T2D mice”
1:29 PM
高糖处理后的外泌体造成损伤
✎ NOTE
“we generated SC-Exos with reduced miR-27a”
1:31 PM
“Schwann cells were transfected with an miR-27a inhibitor (mmu-miR-27a-3p, miRCURY LNA miR inhibitor; Exiqon) or a scrambled control (miRCURY LNA miR inhibitor control; Exiqon) using electroporation”
1:31 PM
“*db/db* mice treated with SC-Exos exhibited significantly improved MCV and SCV in the sciatic nerve, thermal latency (plantar test), and mechanical latency (von Frey test) starting at 4 weeks, which were maintained during the 8 weeks of treatment”
2:00 PM
“SC-Exos on DPN is specific because FC-Exos did not improve NCVs and the mechanical and thermal sensitivity”
2:00 PM
“*db/db* mice exhibited a significant reduction of PGP9.5-positive sensory IENF density, whereas the SC-Exo treatment significantly increased IENF density in *db/db* mice”
2:01 PM
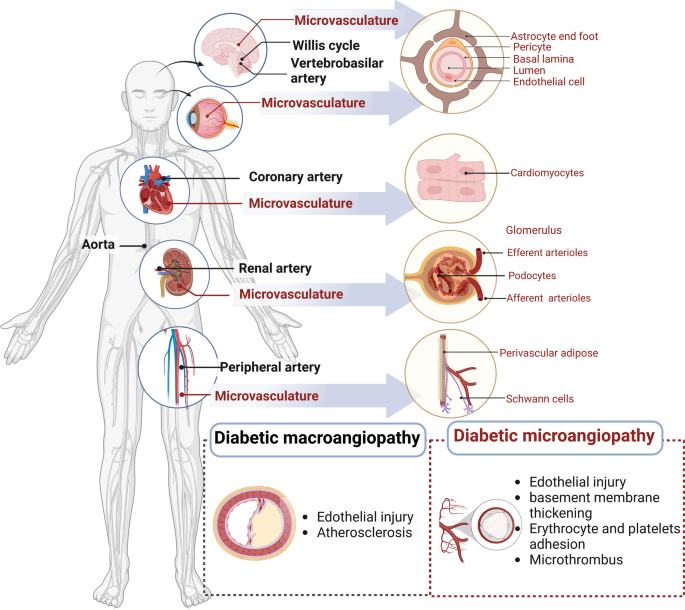
Diabetic Vascular Diseases: Molecular Mechanisms and Therapeutic Strategies
Nature
“糖尿病泛血管病变(DPD)是指糖尿病患者心、脑、肾、眼和外周系统的各种大小血管(包括大血管和微血管)发生动脉粥样硬化这一共同病理变化的临床综合征”
3:36 AM
“Diabetic panvascular disease (DPD) is a clinical syndrome in which vessels of various sizes, including macrovessels and microvessels in the cardiac, cerebral, renal, ophthalmic, and peripheral systems of patients with diabetes, develop atherosclerosis as a common pathology.”
3:39 AM
“Aggressive glycemic control combined with early comprehensive vascular intervention is the key to prevention and treatment”
3:46 AM
早期血管干预
✎ NOTE
“Pathological manifestations of DPDs usually manifest macrovascular atherosclerosis, as well as microvascular endothelial function impairment, basement membrane thickening, and microthrombosis”
3:46 AM
小血管内皮功能损伤
✎ NOTE
“endothelial barrier damage”
3:56 AM
“Microvascular function can affect collateral circulation in macrovessels[56](https://www.nature.com/articles/s41392-023-01400-z#ref-CR56),[57](https://www.nature.com/articles/s41392-023-01400-z#ref-CR57) and increase the risk of stroke[58](https://www.nature.com/articles/s41392-023-01400-z#ref-CR58) as well as a poor prognosis.[59](https://www.nature.com/articles/s41392-023-01400-z#ref-CR59),[60](https://www.nature.com/articles/s41392-023-01400-z#ref-CR60),[61](https://www.nature.com/articles/s41392-023-01400-z#ref-CR61) Neurons injury,[62](https://www.nature.com/articles/s41392-023-01400-z#ref-CR62) Alzheimer’s like pathologies,[63](https://www.nature.com/articles/s41392-023-01400-z#ref-CR63) and abnormal activity of neurotransmitter receptors[64](https://www.nature.com/articles/s41392-023-01400-z#ref-CR64) are also closely associated with cerebrovascular lesions, and jointly cause brain function impairment in patients.”
4:01 AM
“Not only DM but also pre-DM can promote the development of dementia.”
4:02 AM
“Endothelial dysfunction and cardiovascular outcome in asymptomatic patients with type 2 diabetes: a pilot study.”
6:33 AM
“Intracranial pathological changes of microangiopathy include endothelial dysfunction”
6:33 AM
“The expression of vascular endothelial growth factor (VEGF) and endothelin nitric oxide synthase (eNOS) are decreased in DE, which impairs cerebral artery endothelial function and results in decreased vascular autoregulatory response.”
6:34 AM
“Blood brain barrier injury in diabetes: unrecognized effects on brain and cognition”
6:34 AM
“Disturbance of carbohydrate metabolism can cause an intracranial energy metabolism imbalance and promote lesion development”
6:36 AM
“he accumulation of AGEs also affects various cellular constituents of the BBB, resulting in increased BBB permeability and cognitive impairment”
6:39 AM
“Vascular endothelial dysfunction further promotes the production of inflammatory mediators that disrupt the BBB,[59](https://www.nature.com/articles/s41392-023-01400-z#ref-CR59),[63](https://www.nature.com/articles/s41392-023-01400-z#ref-CR63),[64](https://www.nature.com/articles/s41392-023-01400-z#ref-CR64),[100](https://www.nature.com/articles/s41392-023-01400-z#ref-CR100) which exposes the brain parenchyma to potentially neurotoxic proteins”
6:40 AM
“Glutamate receptors, including *N*-methyl-d-aspartic acid receptors (NMDA), may regulate neurogenesis and synaptic plasticity.[106](https://www.nature.com/articles/s41392-023-01400-z#ref-CR106),[107](https://www.nature.com/articles/s41392-023-01400-z#ref-CR107) Upregulation of NMDA receptors had beneficial effects on learning and memory in diabetic rats”
6:55 AM
“The main therapeutic approaches target brain microvascular endothelium and the BBB, microvascular function, neuroinflammation, and antiplatelet agents”
6:56 AM
“Extracellular vesicles have recently attracted interest,[150](https://www.nature.com/articles/s41392-023-01400-z#ref-CR150) because they are essentially exosomes and particles[151](https://www.nature.com/articles/s41392-023-01400-z#ref-CR151) that transport miRNA,[152](https://www.nature.com/articles/s41392-023-01400-z#ref-CR152) mRNA,[153](https://www.nature.com/articles/s41392-023-01400-z#ref-CR153),[154](https://www.nature.com/articles/s41392-023-01400-z#ref-CR154) and proteins,[155](https://www.nature.com/articles/s41392-023-01400-z#ref-CR155) and might serve as early biomarkers of DKD.”
7:01 AM
“Streptozotocin induced in C57BL/6 mice develop microangiopathy in various organs at 4‒20 (mostly 8‒10) weeks after the onset of DM”
7:03 AM
“At 12‒20 weeks of DM, late panvascular disease can occur, with advanced vasculopathy of the heart, retina, or brain”
7:06 AM
“Diabetic macroangiopathy does not develop spontaneously in rats after DM modeling; rather, it is generally induced through specific diet control or vascular occlusion of the DM model rats”
7:06 AM
“Rodents have different lipoprotein metabolism from humans and are highly resistant to AS”
7:07 AM
“after simply constructing animal models of diabetes, studies on microangiopathy and macroangiopathy in the same models are scant”
7:07 AM
“Streptozotocin induced in C57BL/6 mice develop typical microangiopathy mostly at 8‒10 weeks after the onset of DM and develop advanced microangiopathy at 12–16 weeks”
7:14 AM
“abnormalities in cellular energy metabolism affect macrovascular and microvascular lesions,[361](https://www.nature.com/articles/s41392-023-01400-z#ref-CR361),[362](https://www.nature.com/articles/s41392-023-01400-z#ref-CR362),[363](https://www.nature.com/articles/s41392-023-01400-z#ref-CR363) including abnormalities in substrate delivery to vascular EC or target organ cells (e.g., cardiac myocytes, thylakoid cells in glomeruli, and neurons and Schwann cells in peripheral nerves), conversion of the ratio of cell-specific fuel sources between glucose intermediates, fatty acids, and amino acids, changes in respiratory chain protein function, and uncoupling of respiratory chains”
8:01 AM
“The “unification hypothesis”[226](https://www.nature.com/articles/s41392-023-01400-z#ref-CR226) suggests that several seemingly independent biochemical pathways that are overactivated in diabetes are actually caused by excessive intracellular glucose flux”
8:02 AM
“Amino acid metabolism also affects oxidative stress in EC via the arginine metabolic pathway.[407](https://www.nature.com/articles/s41392-023-01400-z#ref-CR407) Vascular protective NO is produced via endothelial-type nitric oxide synthase (eNOS).[408](https://www.nature.com/articles/s41392-023-01400-z#ref-CR408),[409](https://www.nature.com/articles/s41392-023-01400-z#ref-CR409) In vitro experiments, arginine deficiency leads to EC eNOS dysfunction.[410](https://www.nature.com/articles/s41392-023-01400-z#ref-CR410) Elevated arginase levels lead to L-arginine depletion, decreased output of NO, increased ROS, and impaired endothelium-dependent vasodilation”
9:02 AM
“The latest drugs in development are ARIs, tyrosine phosphatase 1B inhibitors, PPAR-γ agonizts, regulators of the glucagon system, and mitochondrial energy modulators. Antisense oligonucleotides and monoclonal antibodies are widely developed”
9:15 AM
“Exosomes derived from Schwann cells ameliorate peripheral neuropathy in type 2 diabetic mice.”
9:16 AM
“miRNA-based studies of diagnosis or regulation have found that miR-21 plays an important role in diabetic vascular complications”
9:20 AM
“New technologies such as induced pluripotent stem cells should be developed to enrich experimental findings of DPD and construct model human blood vessel organoids”
9:21 AM
“Multi-omics analysis of diabetic heart disease in the db/db model reveals potential targets for treatment by a longevity-associated gene”
9:21 AM

Reprogramming Astrocytic NDRG2/NF-κB/C3 Signaling Restores the Diabetes-Associated Cognitive Dysfunction
Tao Jiang
“enrichment of neuronal synaptic plasticity genes—*Syt 1, Manf, Syp, and Bdnf*—was observed in module 1”
1:14 AM
“The expression levels of excitatory postsynaptic density marker PSD-95 and presynaptic density marker synaptophysin (SYP) were decreased in diabetic compared to those in non-diabetic mice”
1:17 AM
“the frequency of mEPSCs were abnormally elevated in diabetic compared to non-diabetic mice”
1:17 AM
“The transcriptomic WGCNA revealed that astrocytic and oligodendrocytic genes—*Lcn2*, *Ndrg2*, and *Mobp*—were enriched in module 2”
1:18 AM
“differences in cognitive function between diabetic and normal patients were assessed”
1:43 AM
“We collected the serum and metabolic indicators from thirteen non-diabetic and twenty-seven diabetic patients, then assessed cognitive function using the Digit Symbol Substitution Test (DSST) scoring system”
1:44 AM
“which reflected the negative relationship between astrocytic inflammatory response and neuronal synaptic plasticity in diabetic mice”
1:49 AM
“WGCNA from a large proteomic study on the AD brain and cerebrospinal fluid demonstrated that AD pathology and cognitive dysfunction were correlated with proteins linked to astrocytic and microglial activation”
1:49 AM